
Single-Path Coding: Removing Roadblocks to Productivity
As professional coders, we know it is hard to know everything about every type of coding, from inpatient to outpatient, from long-term care to post-acute

The public comment period ends June 24, 2019 on the CMS proposed changes to CCs and MCCs.
The Centers for Medicare & Medicaid Services (CMS) Inpatient Prospective Payment System (IPPS) proposed changes for acute-care hospitals in the 2020 fiscal year were announced on April 23 and released through the Federal Register on May 3 (the link appears below). Contained within the 520 pages is a discussion of the complication or comorbidity (CC) and major complication or comorbidity (MCC) changes and the associated tables (Excel files) listing the changes.
Per the IPPS proposed rule in the Federal Register, CMS notes that “in our examination of the claims data, we apply the following criteria established in FY 2008 (72 FR 47169) to determine if the creation of a new complication or comorbidity (CC) or major complication or comorbidity (MCC) subgroup within a base MS–DRG is warranted:
In order to warrant creation of a CC or MCC subgroup within a base MS-DRG, the subgroup must meet all five of the above criteria. Some of the key tables to review by health information management (HIM), clinical documentation improvement (CDI), and revenue cycle are the following:
For each secondary diagnosis, CMS measured the impact in resource use for the following three subsets of patients:
Following the above process, CMS then assigned a numeric resource impact value to each diagnosis code. Review page 19235 of the IPPS proposed rule for more details on the analysis that CMS conducted.

So, the first area one would want to look at is the deletions from the CC/MCC lists. There is recommended removal of some pressure ulcer codes from the MCC list, along with a suggestion to move them to CCs. Here is a portion of the ICD-10-CM table regarding pressure ulcers:

For the 153 MCCs on this proposed deletion list, here’s a portion of the ICD-10-CM codes for “initial encounter for closed fracture … proposed to be removed (deleted):”

Then review the table for proposed additions to the MCC list. Do likewise for the CCs.

Per the Federal Register, “as a result of these proposed changes, of the 71,932 diagnosis codes included in the analysis, the net result would be a decrease of 145 (3,244 to 3,099) codes designated as an MCC, a decrease of 837 (14,528 to 13,691) codes designated as a CC, and an increase of 982 (55,142 to 54,160) codes designated as a non-CC.
This comparison chart can be located on page 19236 of the Federal Register version, as well as other information regarding the proposed changes to the CC/MCC list.

There is also a proposal that neoplasm codes and several acute myocardial infarction codes no longer be used as a secondary diagnosis (removing them as MCCs and making them CCs).
It would be very helpful for your facility or organization to run some diagnosis frequency data reports on several of these specific CC/MCC (ICD-10-CM codes) that are being removed to see what the impact to your inpatient case mix could be. The impact may be less than anticipated due to having multiple CC/MCCs on a given encounter, but this is worth a look.
CMS is asking for public comments on each of the MS-DRG classification proposed changes, as well as the other proposals to maintain certain existing MS-DRG classifications discussed in this proposed rule. When submitting comments, refer to file code CMS-1716-P. CMS will accept comments in the following manner:
Please allow enough time for mailed comments to be received before the close of the comment period.
Reference: https://www.cms.gov/Medicare/Medicare-Fee-for-Service-Payment/AcuteInpatientPPS/FY2020-IPPS-Proposed-Rule-Home-Page-Items/FY2020-IPPS-Proposed-Rule-Tables.html?DLPage=1&DLEntries=10&DLSort=0&DLSortDir=ascending; https://www.cms.gov/Medicare/Medicare-Fee-for-Service-Payment/AcuteInpatientPPS/FY2020-IPPS-Proposed-Rule-Home-Page-Items/FY2020-IPPS-Proposed-Rule-Regulations.html?DLPage=1&DLEntries=10&DLSort=0&DLSortDir=ascending


As professional coders, we know it is hard to know everything about every type of coding, from inpatient to outpatient, from long-term care to post-acute
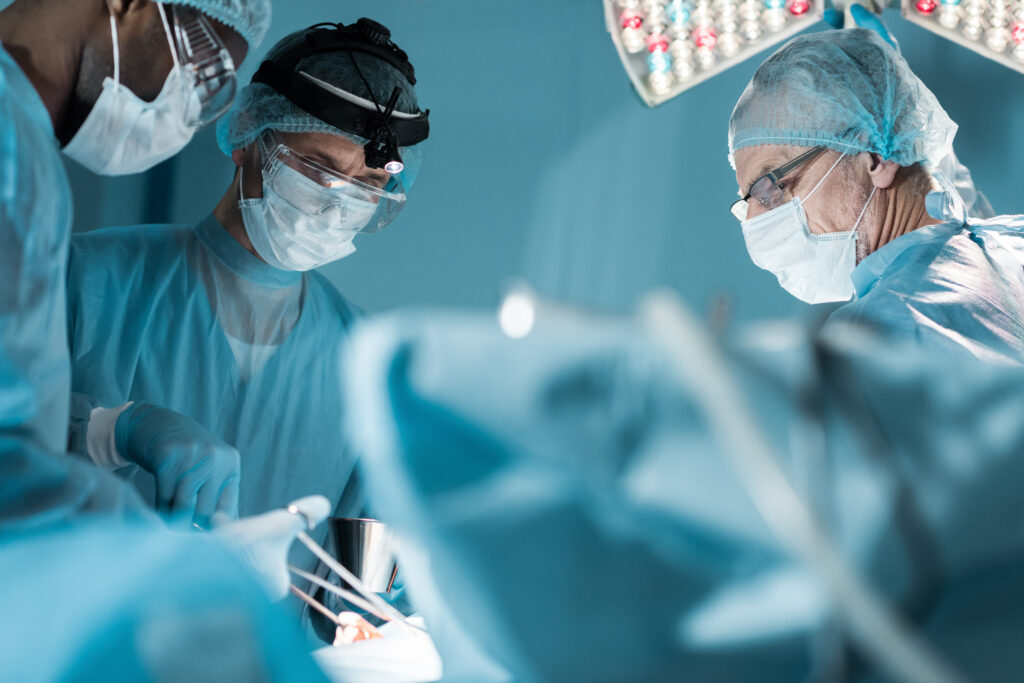
The Inpatient Prospective Payment System (IPPS) Proposed Rule for the 2027 fiscal year (FY) signals another major acceleration in Medicare’s transition toward mandatory value-based care.
Please log in to your account to comment on this article.

Breast biopsy procedures may be clinically straightforward but accurately translating them into compliant billing can be anything but. In this focused webcast, Shawn Blackburn, CPC, CPMA, CIC, CRC, CCS-P breaks down how imaging guidance, lesion count, laterality, and payer expectations all impact how these procedures should be reported. Through clear explanations and real-world scenarios, you’ll gain practical insight into aligning clinical workflows with billing requirements, avoiding common pitfalls, and ensuring your documentation supports accurate reimbursement and compliance.

Gain clarity and confidence in OB‑GYN coding with this expert‑led webcast featuring Sherri L. Clayton, RHIT, CSS. You’ll learn how to apply global maternity package rules accurately, select the right CPT codes for procedures and visits, and identify documentation gaps that lead to denials. With practical guidance and real examples, this session helps you strengthen compliance, reduce audit risk, and ensure accurate reimbursement for women’s health services.

Uncover essential coding insights with nationally recognized coding authority Kay Piper, RHIA, CDIP, CCS. Through ICD10monitor’s interactive, on‑demand webcast series, Kay walks you through the AHA’s 2026 ICD‑10‑CM/PCS Quarterly Coding Clinics, translating each update into practical, easy‑to‑apply guidance designed to sharpen precision, ensure compliance, and strengthen day‑to‑day decision‑making. Available shortly after each official release.

Uncover critical guidance on the ICD-10-CM/PCS code updates. Kay Piper reviews and explains ICD-10-CM/PCS coding guidelines in the AHA’s fourth quarter 2026 ICD-10-CM/PCS Coding Clinic in an easy to access on-demand webcast.

Traditional utilization management models can no longer keep pace with regulatory shifts, payer scrutiny, and operational pressures. In this webcast, Tiffany Ferguson, LMSW, CMAC, ACM, ACPA-C, introduces an Adaptive Model strategy that modernizes UM through role specialization, technology-driven workflows, and proactive, team-based processes. Attendees will learn how to restructure programs to improve efficiency, strengthen clinical collaboration, and enhance financial performance in a rapidly changing healthcare environment.

Federal auditors are intensifying their focus on inpatient psychiatric facilities, using advanced data analytics to spotlight outliers and pursue high‑dollar repayments. In this high‑impact webcast, Michael Calahan, PA, MBA, Compliance Officer and V.P., Hospital & Physician Compliance, breaks down what regulators are really targeting in IPF-PPS admissions, documentation, treatment and discharge planning. Attendees will learn practical steps to tighten processes, avoid common audit triggers and protect reimbursement and reduce the risk of multimillion-dollar repayment demands.

In this timely session, Stacey Shillito, CDIP, CPMA, CCS, CCS-P, CPEDC, COPC, breaks down the complexities of Medical Decision Making (MDM) documentation so providers can confidently capture the true complexity of their care. Attendees will learn practical, efficient strategies to ensure documentation aligns with current E/M guidelines, supports accurate coding, and reduces audit risk, all without adding to charting time.

Join Ronald Hirsch, MD, FACP, CHCQM for The PEPPER Returns – Risk and Opportunity at Your Fingertips, a practical webcast that demystifies the PEPPER and shows you how to turn complex claims data into actionable insights. Dr. Hirsch will explain how to interpret key measures, identify compliance risks, uncover missed revenue opportunities, and understand new updates in the PEPPER, all to help your organization stay ahead of audits and use this powerful data proactively.
Happy HIP Week! Sign up to win free access to our 2026 Coding Clinic Update Webcast Series! Click here to learn more →
Prepare for the 2025 CMS IPPS Final Rule with ICD10monitor’s IPPSPalooza! Click HERE to learn more
Get 15% OFF on all educational webcasts at ICD10monitor with code JULYFOURTH24 until July 4, 2024—start learning today!
CYBER WEEK IS HERE! Don’t miss your chance to get 20% off now until Dec. 1 with code CYBER25
CYBER WEEK IS HERE! Don’t miss your chance to get 20% off now until Dec. 2 with code CYBER24